NCI: Updates of the Understanding of Gliomatosis Cerebri
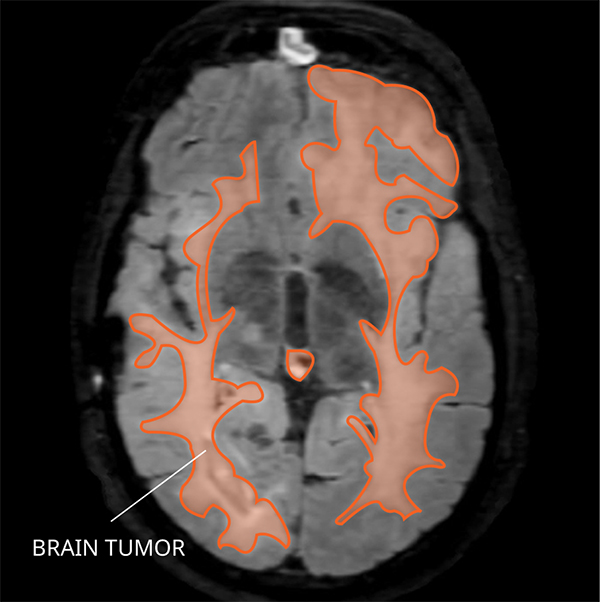
MRI of gliomatosis cerebri in the brain. Credit: NCI-CONNECT Staff
Gliomatosis cerebri is a primary central nervous system (CNS) tumor. This means it begins in the brain or spinal cord. This tumor is no longer recognized as a formal diagnosis, rather gliomatosis cerebri refers to a special pattern of diffuse and extensive growth of glioma cells, invading multiple lobes of the brain. Gliomas of different grade and cell of origin (astrocytes, oligodendrocytes) can grow with this pattern, and very little is understood about the molecular basis of the disease. More research is needed to discover the origin of these tumors and to improve their treatment.
What are the grades of gliomatosis cerebri?
Gliomatosis cerebri are grouped in three grades based on their characteristics.
- Grade II gliomatosis cerebri are mid-grade tumors. This means the tumors have a higher chance of coming back after being removed. They usually have a change in the genes called isocitrate dehydrogenase (IDH).
- Grade III and IV gliomatosis cerebri are malignant (cancerous). This means they are fast-growing tumors that often become resistant to treatment.
Who is diagnosed with gliomatosis cerebri?
Gliomatosis cerebri occur most often in people between the ages of 46 and 53, but can occur at any age. Gliomatosis cerebri occur slightly more often in males than females.
What causes gliomatosis cerebri?
The cause of gliomatosis cerebri are not known.
Where does gliomatosis cerebri form?
Gliomatosis cerebri commonly arises from glial cells in the brain. Glial cells support and insulate neurons and are the most abundant cells in the brain. When seen under a microscope the tumor cells resemble glial cells and involve many areas of the cerebrum. This is why this is named gliomatosis cerebri.

Do gliomatosis cerebri spread?
Gliomatosis cerebri can spread to other areas of the CNS through cerebrospinal fluid (CSF). They can spread quickly and deeply into surrounding brain tissue. They do not spread outside the CNS.
What are symptoms of gliomatosis cerebri?
Symptoms related to a gliomatosis cerebri depend on the tumor’s location and patient’s age. Some possible symptoms include seizures, fatigue, mood changes, changes in thinking and memory, and headaches.
What are treatment options for gliomatosis cerebri?
The first treatment for a gliomatosis cerebri is surgery, if possible. The goal of surgery is to obtain tissue to determine the tumor type and remove as much of the tumor as possible without causing more symptoms for the person. Surgery is usually limited to a biopsy, as there is not a central mass for removal.
After surgery, there is no standard treatment for gliomatosis cerebris. Other treatments may include radiation, chemotherapy, or clinical trials. Treatments are decided by the patient’s healthcare team based on the patient’s age, remaining tumor after surgery, tumor type, and tumor location. This tumor type may respond well to radiation therapy, but patients should discuss the full risks and benefits with their healthcare team, as radiation to a large volume of brain tissue puts normal brain tissue at risk for problems. Chemotherapy is also a treatment that may be recommended during radiation, after radiation is completed, or if the tumor recurs after initial treatment. Temozolomide is a drug that is often used, as this is the therapy for astrocytic type tumors. Clinical trials, with new chemotherapy, targeted therapy, or immunotherapy drugs, may also be available and can be a possible treatment option.
What do gliomatosis cerebri look like on an MRI?
Gliomatosis cerebri usually appear abnormal in three or more lobes of the brain.
- Type 1 shows no obvious mass, but a widespread tumor pattern or a fluffy looking abnormality.
- Type 2 shows a widespread fluffy looking tumor pattern, but also a tumor mass.
Gliomatosis cerebri is diagnosed based on imaging, instead of pathology like most other tumor types.
Posted: September 17, 2018
This content is provided by the National Cancer Institute (www.cancer.gov)
Syndicated Content Details:
Source URL: https://www.cancer.gov/publishedcontent/syndication/1120676.htm
Source Agency: National Cancer Institute (NCI)
Captured Date: 2018-09-17 21:10:25.0
